Топ 4 популярных медицинских носимых

Следующие 10 лет ознаменуют собой план Организации Объединенных Наций «Десятилетие здорового старения».
И нам нужны самые продаваемые носимые устройства для удовлетворения растущего спроса:
1. Умные часы артериального давления

- Мониторинг БП:Чтобы проверить, просто нажмите кнопку, держите руку над сердцем, и манжета автоматически надуется и сдуется сама по себе. Когда это сделано, вы можете увидеть показания вашего кровяного давления на экране.
- Отслеживание сна: Функция сна не просто отслеживает ваш сон. Это также поможет вам создать расписание и идеальный режим сна, чтобы вы могли достичь своих целей сна.
- Отслеживание тренировок: Бег в помещении, бег на открытом воздухе, ходьба в помещении, вы называете это-у SmartWatch MedAsia есть тренировка, чтобы ваши эндорфины начали работать. Начальная линия находится на вашем запястье.
- Отслеживание калорий: Такие данные, как шаги, калории, скорость и т. Д. Можно получить для каждого упражнения. Упражнение более научное, а запись данных более точная.
2. Непрерывный мониторинг уровня глюкозы

- Точное измерение уровня сахара в крови в течение всего дня с автоматической записью диаграмм.
- Легко и удобно носить, компактный размер.
- Всесторонние отчеты анализа сахара в крови позволяют более точное лечение врачами и более легкое управление уровнем сахара в крови.
- Возможность удаленного просмотра данных о сахаре в крови семьи и друзей.
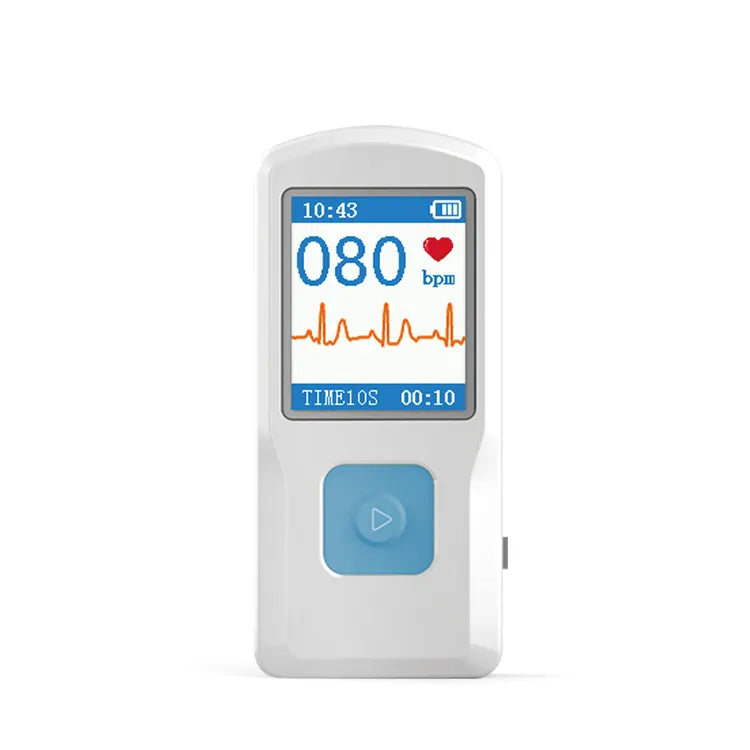
3. Портативный монитор ЭКГ
- Подходит как для индивидуального, так и для семейного использования, портативный дизайн.
- Эффективно помогает предотвратить сердечно-сосудистые заболевания и снизить риски.
- Интеллектуальный дизайн позволяет удаленное управление здоровьем через мобильное приложение.
- Автоматизированное измерение, хранение ЭКГ, загрузка данных, выводы о здоровье и консультации врачей.
4. All-In-One Arm Монитор артериального давления
- Компактный, универсальный и ультратонкий универсальный дизайн для удобства и портативности.
- Следите за своим артериальным давлением легко, где и когда вам нужно.
- Легко оборачивается вокруг плеча без проводов, обеспечивая точные измерения.
- Бесшовное подключение Bluetooth к мобильному приложению позволяет отслеживать артериальное давление в реальном времени.
- Обеспечивает всесторонние показания, включая диастолическое, систолическое и частоту пульса.
Развитие и проблемы медицинских носимых
Инвестиции и инновации необходимы для решения проблемы распространенности общих состояний здоровья, часто называемых «тихими пандемиями», таких как болезнь Альцгеймера, высокое кровяное давление, диабет и депрессия. Эти условия требуют различных измерений и вариантов лечения. Хотя исследования этих условий обширны, они продолжают значительно влиять на здоровое старение.
В соответствии с десятилетней стратегией Организации Объединенных Наций предпринимаются усилия по улучшению условий жизни на основе скоординированных действий, направленных на решение задач, связанных с возрастом и старением, с уделением особого внимания данным и инновациям. Данные считаются ценным товаром в здравоохранении, часто называемым новой кровью.
Поэтому сбор данных для улучшения измерения и лечения имеет решающее значение в течение этого десятилетия глобальных усилий по улучшению различных состояний здоровья.
Примечательной тенденцией в области данных и диагностики является смещение места измерения и лечения. Цифровые технологии, такие как носимые устройства, позволяют сместить парадигму в сторону «больниц без стен». Эта концепция согласуется с идеей независимой жизни, позволяя пациентам оставаться в своей повседневной среде без необходимости частых посещений больниц или клиник. Этот подход предлагает два непосредственных преимущества: он снижает нагрузку на пациентов, которые могут иметь ограничения в мобильности и транспортировке, и оптимизирует время врачей, позволяя им сосредоточиться на людях, требующих личного внимания.
Кроме того, удерживая пациентов дома, их регулярные привычки могут обеспечить более информативные данные по сравнению со спорадическими оценками в клинических условиях. Носимые технологии играют важную роль в этом контексте, обеспечивая длительный и удаленный сбор данных, что приводит к лучшему пониманию и персонализированным подходам к здравоохранению.

Продвижение носимых в здравоохранении
Традиционные клинические визиты для сбора данных в клинической помощи ограничены захватом одного момента времени или коротких временных рамок. Эти визиты создают материально-технические и финансовые проблемы для участников, особенно для лиц с тяжелыми заболеваниями.
Тем не менее, появление носимых устройств позволяет осуществлять непрерывный удаленный мониторинг данных о здоровье пациентов, пока они живут своей повседневной жизнью. Эти инновационные измерения дают ценную информацию о физиологии и результатах заболевания. Кроме того, эта новая эра данных, генерируемых носимыми устройствами, позволяет использовать цифровое фенотипирование, которое включает в себя количественную оценку отдельных пациентов с использованием мультимодальных данных от персональных цифровых устройств и способствует развитию цифровых двойников для точной медицины.
Согласно исследованию, проведенному Masanneck et al. Использование носимых устройств в клинической помощи при хронических неврологических расстройствах, включая эпилепсию, рассеянный склероз, болезнь Альцгеймера и болезнь Паркинсона, значительно эволюционировало.
Они проанализировали зарегистрированные испытания и обнаружили, что относительная частота клинической помощи с использованием носимых устройств увеличилась с 0,7% в 2010 году до 11,4% в 2020 году. Кроме того, Kaiser Associates прогнозирует, что к 2025 году носимые датчики будут включены в 70% клинической помощи. Масаннек и др. Также наблюдался сдвиг в типах используемых цифровых измерений с переходом от простых методов отслеживания, таких как двигательные функции и схемы упражнений, к более сложным мерам, таким как отслеживание речи и познания.
Эти результаты подчеркивают растущее внедрение цифровых технологий здравоохранения (DHT) в неврологических испытаниях и расширение цифровых измерений для конкретных заболеваний.

Преодоление проблем и расширение доступа
Носимые изделия произвели революцию в ландшафте клинической помощи, позволяя им проходить в любом месте и в любое время. Децентрализованные и виртуальные испытания оказались полезными для пациентов, поскольку они уменьшили нагрузку, связанную с участием в испытаниях, такую как время и затраты на проезд, а также ускорили темпы клинических исследований.
Тем не менее, важно признать, что испытания с использованием носимых устройств могут непреднамеренно создать различия и неудобства для определенных групп, особенно для тех, кто имеет ограниченный доступ к Интернету или недостаточную технологическую грамотность. В докладе Lancet и Financial Times «Управление будущим здравоохранения 2030: рост в цифровом мире» подчеркивается необходимость инвестиций в средства цифровой трансформации в общественном здравоохранении и всеобщем охвате услугами здравоохранения, в соответствии с дорожными картами стран и работы по созданию надежной национальной цифровой инфраструктуры.
Существующий цифровой разрыв усугубляет отключение от онлайновых услуг, что еще больше усугубляет проблемы, с которыми сталкиваются уязвимые группы населения. Преодоление этого разрыва требует создания надежной и доступной интернет-инфраструктуры в особо уязвимых районах.
Устранение препятствий для доступа к децентрализованной и виртуальной клинической помощи имеет важное значение для обеспечения равноправного участия и максимизации потенциальных преимуществ носимых устройств. Инвестируя в инфраструктуру и продвигая цифровую инклюзивность, мы можем создать более инклюзивную и доступную среду для всех участников, в конечном итоге продвигая область медицинских исследований.
Верификация участников и обеспечение точности данных
Аутентификация участников создает особые трудности в контексте удаленного сбора данных в виртуальной клинической помощи. Использование носимых устройств лицами, отличными от предполагаемых субъектов, представляет значительный риск для надежности данных, собранных в ходе испытаний. Биометрические методы аутентификации, такие как сканеры отпечатков пальцев или радужной глаза, уже используются для точной идентификации пациентов в клиническом лечении на месте.
Тем не менее, эти технологии еще предстоит широко использовать в виртуальной клинической помощи, что делает их потенциальной ключевой инновацией в этой области. Недавние исследования успешно продемонстрировали, что непрерывно получаемые данные сами по себе могут использоваться для непрерывной аутентификации. Например, модели искусственного интеллекта (ИИ) могут идентифицировать конкретных пользователей, анализируя биометрические данные, связанные с передвижением и частотой сердечных сокращений, собранные с помощью носимых на запястье носимых устройств.
Несмотря на доступность этой технологии, необходимо рассмотреть соображения, касающиеся конфиденциальности и удобства использования, до их широкого внедрения в клиническую помощь.
В отличие от сбора данных в традиционных лабораторных условиях, обеспечение качества данных остается одной из наиболее значительных проблем, которые влияют на надежность данных, полученных в реальных сценариях. Артефакты могут возникать из различных источников, включая окружающую среду (например, показания повышенной температуры, когда устройство покрыто одеялом), само устройство или пациента (например, неправильное размещение устройств).
Кроме того, отсутствие полных данных также может оказывать существенное влияние на качество данных, что подчеркивает важность оценки полноты данных. Например, участники могут выбрать не носить датчик запястья во время сна или во время действий, связанных с водой, таких как душ или плавание, если датчик не является водонепроницаемым.
Вывод
Носимые технологии становятся все более популярными в качестве предлагаемых инструментов для использования в современной медицине. Исследования свидетельствуют об их растущем прагматизме и предоставлении объективных данных для более информативного и персонализированного подхода к уходу за пациентами. В целом, носимые устройства предвещают новую эру в оказании медицинской помощи, чтобы преобразовать многие аспекты клинической помощи.
PS: Если вы хотите, чтобы моя команда изготовила ваши собственные медицинские носки, свяжитесь с нами.Insights@medasiagroup.com
МЫ РЕКОМЕНДУЕМ
Похожие статьи
- Подписаться MedInsights
- Подписаться MedInsights
- Подписаться MedInsights
- Подписаться MedInsights
- Подписаться MedInsights